 The University of Michigan establishes its medical school.
The University of Michigan establishes its medical school.
 James B Angell becomes president of U-M. By the 1880s he has set up the first university hospital in the U.S.
James B Angell becomes president of U-M. By the 1880s he has set up the first university hospital in the U.S.
 U-M establishes its third university hospital, the first four-year medical school curriculum in the U.S., and the School of Nursing.
U-M establishes its third university hospital, the first four-year medical school curriculum in the U.S., and the School of Nursing.
George Dock publishes "Some Notes on the Coronary Arteries," in which he makes an antemortum diagnosis of myocardial infarction and describes its pathophysiology.
 Arthur Robertson Cushny publishes a paper on the effects of digitalis on the mammalian heart.
Arthur Robertson Cushny publishes a paper on the effects of digitalis on the mammalian heart.
Cushny authors the first description of atrial fibrillation in man.
 Albion Walter Hewlett is named chair of the Department of Internal Medicine at U-M; his book on clinical pathophysiology is the first in English. Hewlett was an important early physiologic cardiologist.
Albion Walter Hewlett is named chair of the Department of Internal Medicine at U-M; his book on clinical pathophysiology is the first in English. Hewlett was an important early physiologic cardiologist.
Hewlett publishes "The Clinical Value of the Electrocardiogram," correctly predicting the importance of electrocardiography.
 Frank Norman Wilson writes about a case of anomalous atrioventricular excitation, known today as Wolff-Parkinson-White syndrome.
Frank Norman Wilson writes about a case of anomalous atrioventricular excitation, known today as Wolff-Parkinson-White syndrome.
U-M researchers introduce the electrocardiogram (EKG) to American physicians.
Frank Norman Wilson first designs and then continuously upgrades a Heart Station aimed at researching cardiovascular pathologies.
A new hospital is built in which the Heart Station is established especially to study cardiology.

 John Alexander creates the first formal Thoracic Surgery Residency in the United States at the University of Michigan.
John Alexander creates the first formal Thoracic Surgery Residency in the United States at the University of Michigan.
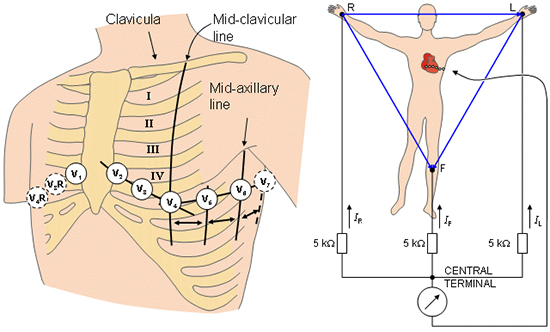
Frank Norman Wilson and colleagues publish a paper in which theoretical values for electromotive forces are derived with bipolar leads; the concept of the central terminal is born.
 Frank Norman Wilson and colleagues publish a series of papers, including one in which they note that atrial fibrillation may be the first and only symptom of thyrotoxicosis.
Frank Norman Wilson and colleagues publish a series of papers, including one in which they note that atrial fibrillation may be the first and only symptom of thyrotoxicosis.
The American Board of Internal Medicine approves four types of subspecialties for certification in internal medicine, including cardiology.
 Frank Norman Wilson and Franklin Johnston report on a patient with angina pectoris and deduce that nicotine from cigarette smoke may play a role.
Frank Norman Wilson and Franklin Johnston report on a patient with angina pectoris and deduce that nicotine from cigarette smoke may play a role.
Frank Norman Wilson's electrocardiography system incorporating the central terminal is formally adopted, thus paving the way for today's 12-lead electrocardiogram.
John Alexander successfully resects an aneurysm caused by coarctation of the aorta.
 Cameron Haight ligates a patent ductus arteriosus.
Cameron Haight ligates a patent ductus arteriosus.
 Sibley Hoobler opens a hypertension follow-up clinic, one of the first in the country. First to recognize that hypertension and elevated lipids are frequently seen together, Hoobler added a full-time lipids expert to the hypertension unit. Hoobler is also credited with coining the term "angiotensin", brokering agreement between competing experts who favored either the term "angiotonin" or "hypertension".
Sibley Hoobler opens a hypertension follow-up clinic, one of the first in the country. First to recognize that hypertension and elevated lipids are frequently seen together, Hoobler added a full-time lipids expert to the hypertension unit. Hoobler is also credited with coining the term "angiotensin", brokering agreement between competing experts who favored either the term "angiotonin" or "hypertension".
 Franklin Davis Johnston initiates the U-M cardiology fellowship training program.
Franklin Davis Johnston initiates the U-M cardiology fellowship training program.
 Herbert Sloan and associates perform a successful repair of an aortic aneurysm.
Herbert Sloan and associates perform a successful repair of an aortic aneurysm.
Franklin Davis Johnston becomes head of the Heart Station.
Cameron Haight inaugurates a closed mitral valvulotomy procedure.
Herbert Sloan and associates repair a coarctation.
Herbert Sloan performs U-M's first open heart surgery.
 Marion (Bill) DeWeese places the first vena cava sieve to prevent pulmonary embolism.
Marion (Bill) DeWeese places the first vena cava sieve to prevent pulmonary embolism.
DeWeese performs the world's first aortorenal bypass.
 Richard D. Judge and Joe D. Morris implant a pacemaker transthoracically.
Richard D. Judge and Joe D. Morris implant a pacemaker transthoracically.
Herbert Sloan and colleagues report on results from 600 open-heart surgeries.
Sloan performs the world's first successful correction of truncus arteriosus as well as the first successful correction of total anomalous pulmonary venous return.
An adult cardiac catheterization laboratory with cineangiography is constructed at University Hospital.
U-M's first coronary care unit opens.
The landmark report "Smoking and Health: Report of the Advisory Committee to the Surgeon General of the U.S." is published, detailing the negative health effects of tobacco. The committee includes Chairman of the U-M Department of Pharmacology Maurice H. Seevers.
 Benedict Lucchesi, a cardiovascular pharmacologist, demonstrates the addictive properties of nicotine and shows that its systemic administration can reduce the frequency of cigarette smoking.
Benedict Lucchesi, a cardiovascular pharmacologist, demonstrates the addictive properties of nicotine and shows that its systemic administration can reduce the frequency of cigarette smoking.
The heart lung machine developed by U-M cardiologist Herbert Sloan and U-M engineer Richard Sarns, is used in the first human heart transplant in Cape Town, South Africa.
 Donald Kahn performs U-M's first coronary artery bypass graft surgery as well as the first heart transplant, the world's first having been performed in December, 1967.
Donald Kahn performs U-M's first coronary artery bypass graft surgery as well as the first heart transplant, the world's first having been performed in December, 1967.
Benedict Lucchesi demonstrates the role of glucagon as an antidote to restore cardiac contractility in hearts depressed by beta-adrenergic blockade.
Park Weed Willis III replaces Franklin Johnston as chief of cardiology; he and coworkers also are among the first to note the familial occurrence of mitral valve prolapse.
 Richard Judge collaborates with General Electric to engineer a new telephonic pacemaker monitoring system.
Richard Judge collaborates with General Electric to engineer a new telephonic pacemaker monitoring system.
Richard Lampman establishes the Work Performance Laboratory.
William J. Fry establishes the U-M Division of Vascular Surgery.
Joseph Bookstein publishes the first in a series of landmark papers from a national cooperative study on the radiological aspects of renal artery disease.
Ernie Reynolds publishes "Planning for Cardiac Care: A Guide to the Planning and Design of Cardiac Care Facilities," which would become a major source for facility designers for two decades.
The U-M's Noninvasive Vascular Laboratory is established.
 James Stanley assumes leadership of the Vascular Surgery Section.
James Stanley assumes leadership of the Vascular Surgery Section.
James Stanley publishes the definitive classification of arterial fibrodysplasia.
 Bertram Pitt arrives at U-M as Chief of Cardiology.
Bertram Pitt arrives at U-M as Chief of Cardiology.
Pitt and H. William Strauss publish an influential textbook on nuclear cardiology.
The U-M Cardiac Rehabilitation Program is initiated.
 Robert Bartlett, principal developer of the lifesaving heart-lung technology extracorporeal membrane oxygenation (ECMO) joins the U-M faculty. ECMO uses an artificial heart and lung to support the body for a period of days to weeks, allowing a critically ill patient's own heart or lungs time to rest and recover.
Robert Bartlett, principal developer of the lifesaving heart-lung technology extracorporeal membrane oxygenation (ECMO) joins the U-M faculty. ECMO uses an artificial heart and lung to support the body for a period of days to weeks, allowing a critically ill patient's own heart or lungs time to rest and recover.
James Stanley establishes U-M Vascular Surgery Fellowship, which over the next few decades will train one of eight vascular surgery program directors in America.
 William O'Neill performs U-M's first primary angioplasty.
William O'Neill performs U-M's first primary angioplasty.
 Fred Morady arrives at U-M and quickly establishes it as an internationally recognized electrophysiology research center.
Fred Morady arrives at U-M and quickly establishes it as an internationally recognized electrophysiology research center.
William O'Neill performs the world's first coronary atherectomy.
 Eric Topol joins U-M. Topol and others found the Thrombolysis and Angioplasty in Myocardial Infarction (TAMI) research group, establishing the concept of the multicenter randomized trial.
Eric Topol joins U-M. Topol and others found the Thrombolysis and Angioplasty in Myocardial Infarction (TAMI) research group, establishing the concept of the multicenter randomized trial.
As director of the Coronary Care Unit, John Nicklas initiates an outpatient management program for congestive heart failure.
William Kou observes that flecainide has the potential to induce life-threatening arrhythmias, particularly in the presence of myocardial ischemia.
First total artificial heart employed at the University of Michigan.
The Conrad Jobst Vascular Surgery Research Laboratories are established.
 Elizabeth Nabel and colleagues publish the first report of a transplanted gene expressing a protein in a living animal.
Elizabeth Nabel and colleagues publish the first report of a transplanted gene expressing a protein in a living animal.
 The first Conrad Jobst Lecture is given by Michael DeBakey.
The first Conrad Jobst Lecture is given by Michael DeBakey.
 Edward Bove publishes a new standard for survival in infants undergoing surgery for hypoplastic left heart syndrome.
Edward Bove publishes a new standard for survival in infants undergoing surgery for hypoplastic left heart syndrome.
 Seigo Izumo becomes Chief of Cardiology.
Seigo Izumo becomes Chief of Cardiology.
The Milton Bryant Lectureship is inaugurated.
 Kim Eagle is recruited as Chief of Clinical Cardiology and Director of the Heart Care Program.
Kim Eagle is recruited as Chief of Clinical Cardiology and Director of the Heart Care Program.
Fred Morady performs U-M's first minimally-invasive catheter ablation procedure to correct atrial fibrillation.
Results are published from the landmark PLAC1 (prevastatin limitation of atherosclerosis in coronary artieries) trial, in which U-M was a participating center. The study demonstrated that pravastatin reduces progression of coronary atherosclerosis and myocardial infarction in patients with coronary artery disease and mildly to moderately elevated cholesterol levels.
 Eagle and colleagues form the International Registry of Acute Aortic Dissections, which now includes 43 centers worldwide.
Eagle and colleagues form the International Registry of Acute Aortic Dissections, which now includes 43 centers worldwide.
 Elizabeth G. Nabel becomes the first woman named Chief of Cardiology at U-M. She goes on to become the Director of the National Heart, Lung, and Blood Institute and later President of Brigham & Women's Hospital.
Elizabeth G. Nabel becomes the first woman named Chief of Cardiology at U-M. She goes on to become the Director of the National Heart, Lung, and Blood Institute and later President of Brigham & Women's Hospital.
A publication co-authored by Bertram Pitt describes the design and characteristics of the AVERT trial (Atorvastatin versus Revascularization Treatments) which evaluated aggressive lipid-lowering therapy as an alternative to vascularization procedures in patients with significant coronary artery disease.
 Blue Cross Blue Shield of Michigan launches the Cardiovascular Consortium (BMC2), a collaboration of health care providers in the State of Michigan comprised of four statewide coronary intervention quality improvement projects.
Blue Cross Blue Shield of Michigan launches the Cardiovascular Consortium (BMC2), a collaboration of health care providers in the State of Michigan comprised of four statewide coronary intervention quality improvement projects.
Results of the ELITE (Evaluation of Losartan in the Elderly) Study are published, indicating that losartan can be helpful in elderly CHF patients with an abnormal or normal left ventricular ejection function who are unable to tolerate ACE.
U-M one of 195 centers worldwide to participate in the Randomized Aldactone Evaluation Study (RALES), which demonstrated that spironolactone significantly improves outcomes in patients with severe heart failure.
 Richard Prager arrives at U-M as Professor of Surgery and Head of the Section of Adult Cardiac Surgery.
Richard Prager arrives at U-M as Professor of Surgery and Head of the Section of Adult Cardiac Surgery.
U-M participates in SOLVD — Studies of Left Ventricular Dysfunction — a group of NIH-funded projects including a treatment trial, a prevention trial and a registry.
Lead author Bertram Pitt publishes the results of the ELITE II study, which showed no significant differences in the effects of losartan compared with captopril on mortality in patients with symptomatic heart failure.
Richard Prager is named Project Director of the Michigan Society of Thoracic and Cardiovascular Surgeons (MSTCVS) Quality Collaborative, whose goal is improving the care of adult cardiac and thoracic surgery patients.
Under lead author Bertram Pitt, results are published from the QUIET trial (Quinapril ischemic event trial), demonstrating that Quinapril did not significantly reduce the occurrence of ischemic events or the progression of coronary atherosclerosis.
Supported by Blue Cross Blue Shield of Michigan, the Michigan Society of Thoracic and Cardiovascular Surgeons (MSTCVS) Quality Collaborative is formed. The initiative encourages cardiothoracic surgical programs to work together to create a large-scale statewide learning process to improve quality.
 David J. Pinsky recruited to U-M as the institution's seventh Chief of Cardiovascular Medicine.
David J. Pinsky recruited to U-M as the institution's seventh Chief of Cardiovascular Medicine.
 Thomas Wakefield named head of Vascular Surgery Services.
Thomas Wakefield named head of Vascular Surgery Services.
Project Healthy Schools (PHS) is launched. Co-founded by Kim Eagle, PHS is an evidence-driven program that encourages healthy habits in youth through education and environmental change.
Jonathan Haft is appointed Director of U-M's internationally-recognized ECMO program.
U-M's Center for Circulatory Support implants their first CardioWest temporary total artificial heart (TAH-t), one of only five U.S. centers approved to offer the device.
 After a 40-year battle with heart disease, legendary Michigan football coach Glenn E. "Bo" Schembechler dies on the eve of the Michigan-Ohio State game. A champion of cardiovascular medicine at Michigan, Bo was a walking, talking testament to the role of research in helping cardiac patients live longer, healthier lives.
After a 40-year battle with heart disease, legendary Michigan football coach Glenn E. "Bo" Schembechler dies on the eve of the Michigan-Ohio State game. A champion of cardiovascular medicine at Michigan, Bo was a walking, talking testament to the role of research in helping cardiac patients live longer, healthier lives.
The U-M Cardiovascular Center opens its doors, bringing together comprehensive care and game-changing research in a single center. The Center's synergistic model was based on founding leadership representing vascular surgery (James Stanley), cardiology (David J. Pinsky), clinical cardiology (Kim Eagle), and cardiac surgery (Richard L. Prager). Today, the directors include Drs. Eagle, Pinsky and Prager, along with Thomas W. Wakefield (vascular surgery), Stephanie Diccion-MacDonald (nursing) and Linda Larin (chief administrative officer).

James Stanley and Thomas Wakefield establish one of the first three Vascular Surgery residency training programs in the country at U-M.
U-M launches the Artificial Heart Lab. A model for collaboration between engineers, clinicians and biologists, it ushers in a new generation of cardiac tissue engineering.
UMCVC doctors broadcast a minimally invasive endovascular repair live over the world wide web.
 In perhaps the largest single recruitment effort in the Medical School's history, more than two dozen arrhythmia specialists, including physicians, scientists, research staff and students make the move to Michigan from the State University of New York Upstate Medical University. Under the leadership of José Jalife, M.D., and Mario Delmar, M.D., Ph.D., they join existing U-M arrhythmia specialists to form the U-M Center for Arrhythmia Research.
In perhaps the largest single recruitment effort in the Medical School's history, more than two dozen arrhythmia specialists, including physicians, scientists, research staff and students make the move to Michigan from the State University of New York Upstate Medical University. Under the leadership of José Jalife, M.D., and Mario Delmar, M.D., Ph.D., they join existing U-M arrhythmia specialists to form the U-M Center for Arrhythmia Research.
 CVC physicians led by Francis Pagani publish first results of a clinical trial of the HeartMateII®, a next-generation Left ventricular assist device (LVAD), describing its advantages over previous LVADs as a bridge to transplant.
CVC physicians led by Francis Pagani publish first results of a clinical trial of the HeartMateII®, a next-generation Left ventricular assist device (LVAD), describing its advantages over previous LVADs as a bridge to transplant.

 Gilbert Upchurch and G. Michael Deeb establish the Frankel CVC's Multidisciplinary Aortic Program (FCVC-MAP) to improve care and outcomes for patients with aortic disease.
Gilbert Upchurch and G. Michael Deeb establish the Frankel CVC's Multidisciplinary Aortic Program (FCVC-MAP) to improve care and outcomes for patients with aortic disease.
 James Froehlich and colleagues, in partnership with the Blue Cross Blue Shield of Michigan, initiate the Michigan Anticoagulation Quality Improvement Initiative (MAQI2), a statewide registry tracking antico-agulation management.
James Froehlich and colleagues, in partnership with the Blue Cross Blue Shield of Michigan, initiate the Michigan Anticoagulation Quality Improvement Initiative (MAQI2), a statewide registry tracking antico-agulation management.
The U-M Heart Assist Device Program one of the first in the nation to receive Joint Commission certification.
 A U-M patient the first in the U.S. to receive the DuraHeart pump assist device.
A U-M patient the first in the U.S. to receive the DuraHeart pump assist device.
 U-M CVC launches Project My Heart-Your Heart, a novel program for pacemaker reuse in underserved countries.
U-M CVC launches Project My Heart-Your Heart, a novel program for pacemaker reuse in underserved countries.
U-M investigators identify ISL1, the first common gene for congenital heart disease.
The U-M Congenital Heart Center the first hospital in the state and one of the first in the nation approved to implant the Melody transcatheter pulmonary valve in pediatric patients to delay the need for open heart surgery.
The Bicuspid Aortic Valve Registry (BAV), the first in the nation, begins patient enrollment at U-M. The project's goals include better characterization of patients with bicuspid aortic valve disease, assessing the impact of medical interventions and testing for genetic and familial risk of disease.
The Joint Institute for Translational and Clinical Research between U-M and Peking University (PKU) is established to sponsor high-impact collaborative research in pulmonary, cardiovascular and liver disease.
The Study of Exercise Training in Hypertrophic Cardiomyopathy (REST-HCM) launches, assessing the impact of moderate intensity exercise on patients with hypertrophic cardiomyopathy.
 Legendry hypertension researcher and U-M professor emeritus Stevo Julius the first U.S. scientist to receive the Alberto Zanchetti Life Achievement Award from the European Society of Hypertension.
Legendry hypertension researcher and U-M professor emeritus Stevo Julius the first U.S. scientist to receive the Alberto Zanchetti Life Achievement Award from the European Society of Hypertension.
U-M researchers publish results from the non-randomized Evaluation of the HeartWare® HVAD Left Ventricular Assist Device System for the Treatment of Advanced Heart Failure (ADVANCE) study, demonstrating HVAD outcomes comparable to already approved bridge-to-transplant pumps.
U-M Board of Regents approves a new, independent Department of Cardiac Surgery, one of only two new departments created at the Medical School in more than a decade.
U-M one of 40 U.S. sites to join the PIVOTAL study, a landmark clinical trial of the Medtronic CoreValve as a less invasive option to treat aortic stenosis. Michael Deeb and Stanley Chetcuti perform the first transcatheter aortic valve replacement (TAVR) of the valve at U-M soon after it receives FDA approval.
The University of Michigan-Israel Partnership for Research and Education begins its historic collaboration.
Edward Bove is named founding director of the new Department of Cardiac Surgery. This same year, Bove performs his 10,000th surgery.
 The U-M Cardiovascular Research Center (CVRC) opens at the North Campus Research Complex (NCRC). Directed by José Jalife, the CVRC is the new hub for speeding heart and vascular advances into the clinical arena.
The U-M Cardiovascular Research Center (CVRC) opens at the North Campus Research Complex (NCRC). Directed by José Jalife, the CVRC is the new hub for speeding heart and vascular advances into the clinical arena.
The Center's largest research group is the Center for Arrhythmia Research (CAR), which relocates its team of 85 to the NCRC and names Hector Valdivia as its new director. Other components include the Conrad Jobst Laboratories, home to molecular, hematology and cell biology research, medical device testing and vascular surgical training.
U-M and device maker Integrated Sensing Systems develop a wireless, battery-free cardiac implant for congenital heart patients.
The Berguer Lectureship is established.
U-M pioneers use of radiofrequency-based speckle tracking echocardiography to more accurately assess diastolic function, a major cause of heart failure.
U-M participates in the SYMPLICITY HTN-3 trial, studying an investigational renal denervation system for treatment-resistant hypertension.
U-M aerospace engineers develop a heartbeat-powered pacemaker with the potential to eliminate the need for surgical replacement of pacemakers with depleted batteries.
The U-M Cardiovascular Center is renamed the Frankel Cardiovascular Center in recognition of the support received from the Samuel and Jean Frankel Foundation. It ranks among the top such centers in the nation for heart, vascular and stroke care.
One day after receiving FDA approval, U-M is one of the first heart centers in the U.S. to implant the BIOTRONIC Lumax 740DX, a cardiac defibrillator that uses a single lead to sense vital changes in heart rhythm.
The Cardiovascular Health Improvement Project (CHIP) Study launches, building a biorepository of DNA, plasma, serum, and aortic tissue samples and an extensive clinical database of medical and family history information to facilitate scientific discovery. David Pinsky is awarded an NIH T32 training grant to establish a Multidisciplinary Cardiovascular Research Training Program at U-M.
 David Pinsky and Alan Saltiel, director of the U-M Life Sciences Institute, co-direct a partnership with Technion-Israeli Institute of Technology and the Weizmann Institute to focus on heart disease research.
David Pinsky and Alan Saltiel, director of the U-M Life Sciences Institute, co-direct a partnership with Technion-Israeli Institute of Technology and the Weizmann Institute to focus on heart disease research.
A Frankel CVC team performs the first ever implantation of the GORE® TAG® thoracic branch endoprosthesis. The device seals off a hard-to-treat section of the aorta, potentially providing a safe and less invasive alternative to open surgery.
Frankel CVC team the first in nation to use the Edwards SAPIEN device in a landmark transcatheter tricuspid valve replacement.
 The Frankel CVC is one of the nation's first hospitals to use the Medtronic Reveal LINQ Insertable Cardiac Monitor (ICM) System, the smallest implantable cardiac monitoring device available.
The Frankel CVC is one of the nation's first hospitals to use the Medtronic Reveal LINQ Insertable Cardiac Monitor (ICM) System, the smallest implantable cardiac monitoring device available.
The Frankel CVC is one of the first hospitals in the U.S. to implant Medtronic's investigational CoreValve Evolut R "recapturable" heart valve, studying its use in transcatheter aortic valve replacement (TAVR) in patients considered at high risk for open heart surgery.
Thomas Wakefield appointed Director of the U-M Frankel Cardiovascular Center as James Stanley resumes his role as Professor of Vascular Surgery and Associate Chair of the Department of Surgery.
Thomas Wakefield and Sumie Sood receive NIH funding to treat clinical DVT for the first time with an anti-inflammatory approach, using an inhibitor to E-selectin.
Thomas Wakefield and Peter Henke are awarded an NIH T32 training grant for a Vascular Biology Research training program at U-M.
José Jalife is awarded an NIH T32 training grant for a training program in Translational Cardiovascular Research & Entrepreneurship at U-M.
 Himanshu Patel reports the results of a multicenter feasibility trial of the W.L. Gore Thoracic Single Side Branch Endograft after leading the U-M team that first used the new investigational device to treat a thoracic aneurysm.
Himanshu Patel reports the results of a multicenter feasibility trial of the W.L. Gore Thoracic Single Side Branch Endograft after leading the U-M team that first used the new investigational device to treat a thoracic aneurysm.
Senior study author Vallerie McLaughlin publishes data from the largest study ever of pulmonary hypertension, showing that the oral medication Selexipag reduced hospitalizations and worsening symptoms by 40 percent.
U-M is the first hospital in Michigan to release a patient with a total artificial heart while awaiting transplant.
The Frankel CVC is among the first heart centers in the U.S. to use the WATCHMAN device to help prevent stroke in patients with non-valvular atrial fibrillation.
Vallerie McLaughlin is chosen to take part in the Transition From Inhaled Treprostinil to Oral Selexipag in Patients With Pulmonary Arterial Hypertension (TRANSIT-1) research study sponsored by Actelion.
 The Linda R. Larin Fellowship Fund is created to honor the FCVC Director and Associate Hospital Director for Cardiovascular and Neurosciences Programs for her accomplishments in leading patient- and family-centered care initiatives. The Fund will be used to support for fellows, research assistants, students and/or trainees in the Frankel CVC.
The Linda R. Larin Fellowship Fund is created to honor the FCVC Director and Associate Hospital Director for Cardiovascular and Neurosciences Programs for her accomplishments in leading patient- and family-centered care initiatives. The Fund will be used to support for fellows, research assistants, students and/or trainees in the Frankel CVC.
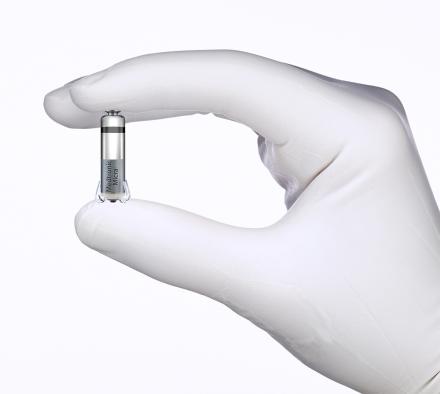 U-M implants the Micra® Transcatheter Pacing System, the world's smallest pacemaker. Placed inside the heart, the Micra is a new option to treat bradycardia.
U-M implants the Micra® Transcatheter Pacing System, the world's smallest pacemaker. Placed inside the heart, the Micra is a new option to treat bradycardia.
U-M begins enrolling patients in a new, expanded indication trial of the CoreValve® Evolut® R System, studying the broader use of transcatheter aortic valve replacement (TAVR) in patients at lower risk of death from valve replacement surgery.
U-M transplant surgeons begin testing the Transmedics Organ Care System (OCS), a box that circulates the donor's blood to the donor heart while it is in transit, allowing it to keep beating outside the body, warm and pumping before transplant.
Robert Neumar and David Pinsky are awarded an NIH K12 grant to develop an emergency critical care research training program at U-M.
The first patient in Michigan ever discharged with a SynCardia temporary total artificial heart (in 2014), receives his heart transplant.
The Frankel CVC opens its new state-of-the-art hybrid operating room, offering life-saving alternatives to open heart surgery.

The Heart Vessel Blood Clinical Trials Support Unit (HVB CTSU) is formed to enhance the performance of cardiovascular and other clinical trials at U-M.
Frankel CVC Director Richard L. Prager elected as President of The Society of Thoracic Surgeons.
The Frankel CVC celebrates the 10-year anniversary of their clinical building.